Mouth Ulcers
Mouth ulcers are a common affliction. They are often referred to as canker sores. They may simply caused by trauma and heal quickly on their own. The recurrent, bothersome form is known as recurrent aphthous stomatitis or simply aphthous ulcers.
Cause - Unknown, though it is believed to be some sort of immune mediated condition. At this time it seems aphthous stomatitis is not caused by any infectious agent (viruses or bacteria) and these ulcers are not contagious. Aphthae can also be manifestations of various systemic diseases such as Bechet's syndrome, HIV, autoimmune disorders, Crohn's disease, and the like.

Common Recurrent Aphthous Stomatitis
Characteristics- These lesions are almost always found on the "loose" tissues of the mout like the cheek, inner lip, tongue, soft palate, floor of mouth, and sometimes the throat. They are usually small, less than one half centimeter in diameter. A reddish halo usually surrounds them. A less common form, major aphthae, can get quite large and take very long to heal. An even rarer form is the herpetiform ulcer, characterized by multiple tiny ulcerations in many parts of the mouth at once, including the firmer gum and palate tissues. Herpetiform ulcers are uncommon and sometimes mistaken for herpes outbreaks (below).
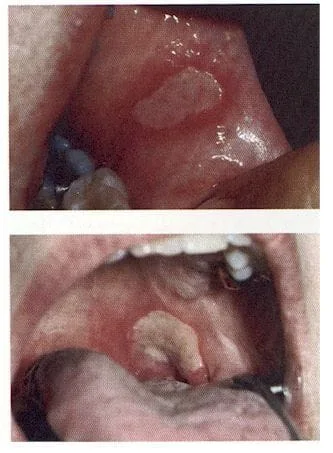
Major Apthae
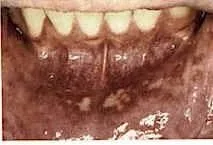
Herpetiform Ulcers
Triggers - Stress, acidic foods, specific foods for the individual, trauma, chemical sensitivities, and the like all can play a role in setting off an attack. Some studies have indicated that toothpastes containing the additive sodium lauryl sulfate (SLS) can trigger attacks in some people. Using an SLS free toothpaste (Biotene, Squigle) has been shown to reduce attacks significantly (50-70 per cent) in susceptible individuals.
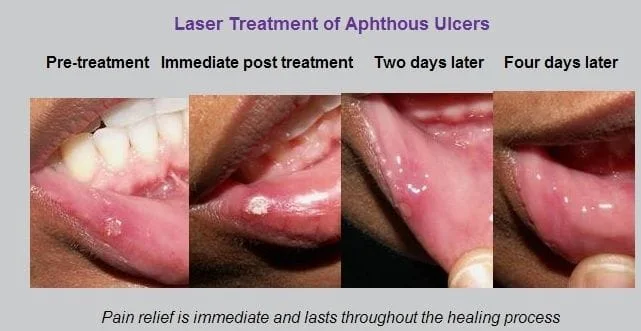
Treatment - There is no cure for aphthous stomatitis. Laser treatments are the most effective, giving immediate pain relief and causing the ulcer to heal in 24-72 hours. The photos above are typical for laser treated aphthae. Pain relief is immediate and lasting; the ulcers heal in two to four days. A dentist applied treatment, Debacterol, gives almost immediate relief and speeds healing. It is an acidic agent which chemically cauterizes the ulcer surface, sterilizing it, and covering the painful nerve endings. Only available as an in office treatment, Debacterol is 90 percent effective in giving immediate and lasting pain relief. Avoiding known triggers is helpful, such as using the SLS free toothpastes mentioned above. A healthy diet with vitamin supplementation is recommended. Excellent oral hygiene, including use of antibacterial rinses (Rx chlorhexidine or OTC Listerine), has been shown to reduce frequency of attacks. Reducing stress is important as well. Topical steroid treatments (Kenalog, Lidex gel, Decadron rinses) are quite useful, reducing the pain and duration of the lesions. Usually a weaker steroid is used first and stronger varieties are attempted until results are found. In severe cases a short course of systemic steroid (prednisone, etc.) may be needed. A new drug Apthasol is on the market and has been shown to have some beneficial effects as well.
Angular Chelitis
Often mistaken for cold sores, this condition is actually a common fungal infection.
Cause - Fungus, candida albicans, which is responsible for most forms of intraoral fungal (yeast) infections.
Characteristics - Cracked fissures appear at the corners of the mouth. Tender tissues are often surrounded by flaky skin. Infection is mild to moderately painful depending on severity.
Triggers - Deep folds at corners of the mouth due to bite collapse, dentures, etc predispose infections but are not necessary. Oppo
Treatment - Antifungal/ anti-inflammatory ointment (Mycolog II) quite effective, healing occurs in a few days. Patient must learn not to lick their lips when the corners crack, avoiding inoculation. Denture wearers often benefit from a new denture, which can open the bite thus eliminating the folds at the corners of the mouth.
Cold Sores
The common cold sore is known as recurrent herpes labialis.

Cause - Herpes Virus. Most people have been exposed to this virus, but only a small percentage suffer from the re
Characteristics - The recurrent form is usually found on the outer lip. There is typically a period for a day or two prior to the outbreak where the person feels itching in the area the outbreak will occur. It takes a week or two to heal, and has a characteristic crusty appearance. Recurrent herpes can occur in the mouth as well. In a non immunocompromised person it is always found on the non-movable tissue of the mouth (gums and hard palate).
The initial infection with the virus is usually asymptomatic, but in some people it can be quite severe. It is known as Primary herpetic gingivostomatitis. The patient's mouth, gums, and throat are covered with painful ulcers. Lymph nodes swell, fever rises, and the person feels generally awful. Primary herpes is usually found in children and sometimes young adults. It is a self limiting syndrome taking from 10 - 14 days to heal. Zovirax can help speed recovery a bit in more severe cases.
Triggers - Trauma, sunburn, stress, illness, cold weather, and the like.
Treatment - Herpes outbreaks are typically self limiting, but some medications can help speed up the healing process. Laser treatments can give immediate pain relief and the lesion will heal in 24-72 hours. The laser therapy is identical to the laser aphthous treatment shown above. An antiviral ointment, Denavir, can help speed healing of lesions. Antiviral medications (pills) like Valtrex or Zovirax can help treat recurrent severe cases. Valtrex got FDA clearance as a treatment for cold sores in the fall of 2002. It is a very easy one day regimen which has been shown to be quite effective. Low doses of Zovirax have been shown to help prevent outbreaks, such as when someone will be in the sun. Avoiding triggers helps, such as wearing sun block and minimizing trauma to the lips. Lysine, an over the counter supplement, will reduce outbreaks in some people.
Another important thing to remember is that these lesions are contagious and one must practice good hygiene during outbreaks. In addition it is possible to infect other parts of your own body if good hygiene practices are not followed. Herpetic whitlow is a painful infection of the fingers and ocular herpes is an eye infection which can become quite severe, even leading to blindness. Do not play with the sores and wash your hands frequently during outbreaks.
Lichen Planus
Lichen planus is a benign dermatologic condition which can occurs in the mouth, sometimes with no apparent skin involvement. Often the mouth lesions will occur prior to generalized skin involvement.
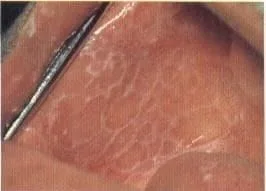
Cause - Unknown. Appears to be a low grade autoimmune reaction. Lichenoid drug reactions are identical to lichen planus and are caused by specific drugs.
Characteristics - Oral lichen planus has a very characteristic appearance. It has a lacy, white pattern of various sizes and can occur anywhere in the mouth, though the inner cheek is the most typical area. The common form is asymptomatic and patients often do not know they even have it unless their dentist points it out to them. The lesions change in size constantly from near remission to full mouth involvement.
Erosive lichen planus is the form where ulcers form within the lesion and can be quite painful. A small percentage of lichen planus patients develop this form of the condition. Ulcerated areas can become quite large and bothersome and episodes can last weeks without treatment. Diagnosis is often made by clinical appearance due to the classic appearance of lichen planus lesion, though biopsy confirmation is often performed.
Lichenoid drug reactions are clinically identical to lichen planus but are actually a specific reaction to a given drug and will resolve if the medication is discontinued.
A very small percentage of chronic oral lichen planus may develop into an oral cancer lesion, so this condition needs to be checked regularly by your dentist.
Triggers - No obvious triggers but stress, drugs in lichenoid form, poor nutrition, and galvanic reactions to fillings have been implicated.
Treatment - No treatment is needed for the asymptomatic form. The ulcerative form can be controlled quite well with the application of topical steroids (Lidex, Decadron).

